Wound care
Most wounds are traumatic, but can also be diabetic neuropathic or vascular. A traumatic wound is suddenly caused by a trauma that compromises the integrity of skin layers. In a healthy person with a good blood supply, the healing process is normal.
1. Neuropathic Wounds
Neuropathy is a condition that affects nerves and many diabetics will suffer the consequences. In a patient with diabetic neuropathy and unstable blood glucose level, the healing process of wounds can be altered and a wound can easily become chronic or get infected.
In the case of neuropathic wounds, pressure points under the feet become places where ulcers may form if there are not correctly managed with an appropriate dressing and a drain.
It is a particular problem because neuropathic patients often do not feel pain, which can easily be the case for a healthy person without neuropathy. As a consequence, the consultation may be delayed, which will greatly increase complication risks.
Daily care under the proper supervision of your podiatrist, who will be able to establish a good treatment plan, will be recommended so that healing is complete and any risk of infection is avoided. During the healing process and then as a precaution, your podiatrist will recommend wearing an orthosis to reduce problematic pressure points under the feet.
2. Arterial wounds
Arterial ulcers can appear in patients with a very bad blood flow in lower limbs. This type of wound is often painful. It looks like a very focal necrosis and is usually located at the tip of the toes. Your podiatrist will be able to evaluate if there is a pedal pulse with a Doppler.
When insufficient blood supply is detected, the patient is recommended a consultation with a vascular specialist so that the arterial blockage is located and proper medical and surgical care is provided.
3. Venous Wounds
Venous wounds form when the venous system is compromised and the venous return towards the heart is inadequate. A venous slowing phenomenon then occurs, which implies a venous stasis. This type of ulcer can be observed mostly on the inside face of the leg, near the ankle.
This type of wound must be treated with proper dressings and compression. The initial step before starting any treatment is to be properly diagnosed by your podiatrist. Afterwards, the follow-up until the end of the healing process is equally essential.
4. Charcot’s Foot
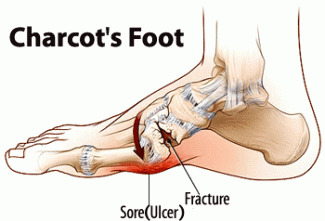
Diabetic neuropathic foot that suffered micro fractures and subluxations over time is called “Charcot’s foot” and is cradle-shaped. Those bone changes are not necessarily linked to injuries or accidents and are often painless in diabetic neuropathic patients. In the first stages of progression, the affected foot is red and very swollen.
This type of foot is seriously managed from the inception of symptoms in order to prevent subsequent subluxations, which could cause pressure points leading to the formation of ulcers under the foot that can also get infected.
The managing requires complete immobilization of the foot. Afterwards, an accommodation orthosis will be required to prevent ulcers at pressure points caused by previous subluxations.
Gatineau Sector
456, boul. de l’Hôpital,
Gatineau, J8T 8M5
Tel. : 819-568-0456

Responsible for the protection of personal information: Dre Lynda Cormier, podiatrist cpogatineau.cpo@gmail.com or (819) 568-0456.

